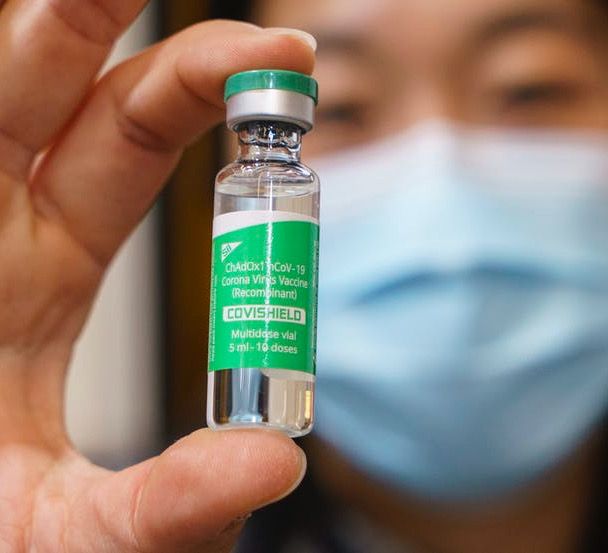
A healthcare worker holds up a vial of the AstraZeneca vaccine at a COVID-19 vaccination clinic in Montréal, on March 18. THE CANADIAN PRESS/Paul Chiasson
Dawn ME Bowdish, McMaster University and Ishac Nazy, McMaster University
Rare but serious blood clots that have been linked the AstraZeneca COVID-19 vaccine have many people — especially those who have already had one dose of the vaccine — looking for information. Here are answers to some key questions.
If I had a first dose of the AstraZeneca COVID-19 vaccine, should I have concerns about safety?
As long as there is a risk, you should always be aware and informed. A risk of very serious harm, including death, does exist, though it is very small: about one in 55,000 for the first dose.
We now have a much better understanding of how to diagnose and treat clotting due to COVID-19 vaccines, called vaccine-induced thrombotic thrombocytopenia, or VITT (also sometimes called vaccine-induced prothrombotic immune thrombocytopenia, or VIPIT) when it does occur. Death rates among people who experience VITT have been estimated at 20 to 50 per cent, but may be improving as knowledge increases. The Public Health Agency of Canada monitors all adverse events following COVID-19 vaccination.
It’s important that everyone who has had the AstraZeneca vaccine understands that it was the right thing to do. It is an excellent and effective vaccine, and being vaccinated is an important act to protect not just yourself, but your community by slowing and eventually stopping the pandemic.
Should I get a second dose of AstraZeneca? If so, when?
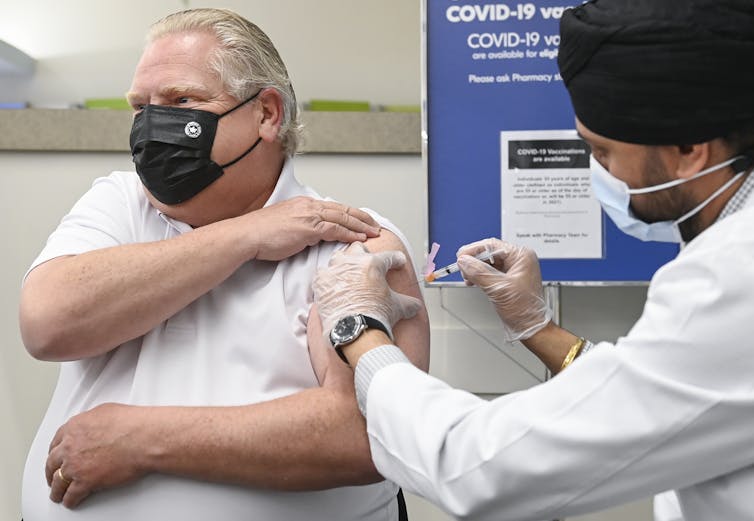
Ontario Premier Doug Ford receives the AstraZeneca COVID-19 vaccine on April 9. THE CANADIAN PRESS/Nathan Denette
Getting the second dose of any two-step vaccine is very important. That’s what cements the memory of the immune response. We know from clinical trials that the first dose does not prevent all infections. It prevents death from infection. The second dose boosts the immune response to almost completely protect you from getting any infection. That second dose also greatly reduces your ability to carry or spread the virus at all.
In terms of timing, evidence is still emerging, but the best guidance regarding AstraZeneca is that a 12- to 20-week gap between first and second doses is ideal, much as it is with most vaccines.
Are the risks different for a second dose?
The risk of a blood clot after a second dose is about one in 600,000, which is one-tenth the risk of clotting after an initial dose. If you were comfortable getting the first dose, you should feel good about going ahead and continuing to help the community bring the pandemic closer to its end. In addition, knowing the symptoms associated with the vaccine-related clots allows for timely recognition and immediate treatment.
How serious a health risk are blood clots that can follow a vaccine?
It’s important that everyone who has had the AstraZeneca vaccine understands that it is an excellent and effective vaccine. THE CANADIAN PRESS/Carlos Osorio
In those very rare cases where blood clots follow vaccination, they can be very serious, even fatal. The good thing is that knowledge is advancing quickly, especially in terms of diagnosing and treating these clots when they do occur.
Earlier in the vaccine rollout, the risk of death in the rare cases of clotting was 60 to 80 per cent. Today, it’s 20 per cent.
At the beginning of the rollout, patients had no way of knowing what a vaccine-related clot was or what to look for. That may have been a key factor in the higher death rate. Now that this issue is known and the symptoms can be identified, the risk of death is much lower. As we’ve progressed in understanding how this issue presents itself, people are being diagnosed and treated much sooner and more effectively.
Is it safe to get a different vaccine for my second dose?
Canada’s National Advisory Committee on Immunization (NACI) recommends that for a second dose, you should stay with a vaccine made with the same technology “platform” as the first. If you first got AstraZeneca, which is a form of viral vector vaccine, it’s recommended that you get it again. If it is not available, Johnson and Johnson is another viral vector vaccine.
If you had a vaccine based on an mRNA technology platform — Pfizer or Moderna — you can have either one of those two for your second dose. More data is emerging, and mixing and matching platforms could ultimately be proven to be safe and effective, but for now, the recommendation is to stay with the same technology.
Update: NACI issued a new recommendation on June 1, 2021. People who received a first dose of AstraZeneca vaccine may now get an mRNA vaccine as a second dose. The discretionary recommendation is based on safety profiles, emerging data on mixing vaccine doses and expert opinion on immune response to different vaccines for the same disease.
Are there any symptoms people should be on the lookout for that may indicate a blood clot?

Pharmacist Barbara Violo arranges all the empty vials of the AstraZeneca COVID-19 vaccine that she has provided to customers at the Junction Chemist pharmacy in Toronto, on April 19. THE CANADIAN PRESS/Nathan Denette
The symptoms of VITT are well documented and include the following, which occur four or more days after vaccination:
- Severe and persistent headaches.
- Severe and persistent blurry vision.
- Leg swelling.
- Difficulty breathing.
- Abdominal pain.
- Bruising beyond the vaccination site.
It is important to seek prompt medical care in these cases. It is also important to note that minor fever, headache, fatigue and pain at the site of the vaccination are common with all vaccines in the first one or two days and are not causes for concern.
Who is at risk from clotting related to the AstraZeneca vaccine?
Clotting events are still so rare that it is very difficult to identify any particular risk factors. Although it appears that a slightly higher number of women have experienced clotting, the number of cases isn’t large enough to accurately assess whether sex might affect risk.
The AstraZeneca vaccine is not recommended for people who have had a previous case of heparin-induced thrombocytopenia, or of rare cerebral venous sinus thrombosis clots. A family history of clotting does not appear to be relevant to vaccine risks since the mechanisms are completely different.

Dawn ME Bowdish, Canada Research Chair in Aging & Immunity, McMaster University and Ishac Nazy, Associate Professor of Medicine and Scientific Director of McMaster Platelet Immunology Laboratory , McMaster University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
"Voices of the RSC” is a series of written interventions from Members and Officials of the Royal Society of Canada. The articles provide timely looks at matters of importance to Canadians, expressed by the emerging generation of Canada’s academic leadership. Opinions presented are those of the author(s), and do not necessarily reflect the views of the Royal Society of Canada.