 KEEPING EVERYONE SAFE: INFECTION PREVENTION & CONTROL IN COVID-19 VACCINE CLINICS
KEEPING EVERYONE SAFE: INFECTION PREVENTION & CONTROL IN COVID-19 VACCINE CLINICS
Jeannette Comeau | April 1, 2021
Jeannette Comeau is Assistant Professor in the Department of Pediatrics at Dalhousie University
Over the past year, the general public has become familiar with the importance of Personal Protective Equipment (PPE) as a means of reducing the spead of COVID 19. However, for those working in Infection Prevention and Control (IPAC), multiple other upstream considerations and controls should be made and observed to ensure that individuals at mass immunization clinics do not contract COVID-19 while administering or receiving the vaccine. In order of effectiveness (and also importance) these are[1]:
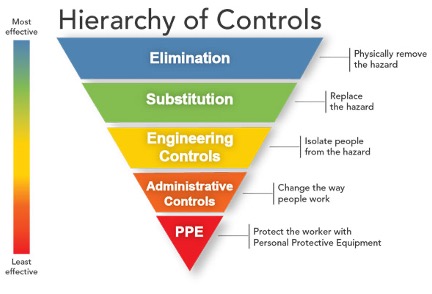 Elimination of Exposure
Elimination of Exposure- Substitution of Activities
- Engineering Controls
- Administrative Controls
- Personal Protective Equipment (PPE)
But how does this hierarchy of controls manifest in practice, and how can we tell if each element is being followed? Let’s work through each concept briefly, and add a checklist that can provide the basis of ensuring these measures are observed all with the ultimate goal of protecting both the vaccination team and the individual receiving the vaccine.
Elimination of Exposure and Substitution of Activities
The most effective measures in the hierarchy of controls are those that contribute to the elimination of the infectious agent. When we reflect on the COVID-19 pandemic measures, the vaccine program itself has the ultimate goal of eliminating the virus from circulation within the community. In the context of immunization clinics, prescreening vaccine recipients well before entering the clinic (and, if they are not well, asking them to return only when they are well again) serves as a form of local elimination.
Engineering Controls
Considerable attention has been placed on ventilation systems when people are indoors, and meeting outside has been recommended when possible. While immunization clinics cannot necessarily be outdoors, they should in large rooms or drive-thru facilities, that provide space for physical distancing and capacity for adequate ventilation both while the vaccine is administered and during the post-immunization observation period.
Additional controls, evaluated by Industrial Engineers, can also be implemented to direct the flow of individuals through the clinic space: ideally unidirectional.
Administrative Controls
Carefully documented policies and procedures should include checklists of the IPAC measures implemented at each site. It is also necessary to have a system in place that screens and tracks both immunizers and immunized, so if an inadvertent exposure occurs, individuals can be quickly notified.
Personal Protective Equipment (PPE)
In a medical setting setting PPE is designed to protect the wearer, and individual users put on and take off their PPE (such as masks, face shields, gowns and gloves) when encountering a potientally contagious patient. It is essential that this is done properly to avoid the possibility of self-contamination. In the context of the pandemic, masking has become an important measure in protecting others, so immunization clinics must have adequate supplies for both the health care providers and those who present for immunization but do not have their own.[JM1] [JC2] [AD3] [AD4]
The American Centre for Disease Control (CDC) has developed comprehensive advice for those providing immunization. This guidance holds true in the Canadian context[2]. If the measures in these checklists are observed, both the public and those working at the clinics will be well protected.
Pre-Vaccination
- Book appointments (rather than walk-ins) to ensure vaccinees do not have to wait when they arrive for their appointment
- Request that vaccinees do not arrive early, and if they do, inform them that they may have to remain in their cars or outside the facility
- Ensure that adequate instructions (in multiple languages) are provided re: expected process, PPE, etc
- Provide pre-screening criteria and simple method of cancellation if the vaccinee becomes ill or exposed to another individual prior to their appointment
- Ensure that they can be rebooked after their quarantine period is completed (14 days), or they are well, as required
At the clinic
- Ensure clinic workers are doing daily self-assessments and not presenting to work if sick
- Have limited entrances for vaccinees, with screening questions asked at entry
- Enforce masking guidelines in compliance with Public Health recommendations (generally masks for those >2 years of age)
- Ensure access to hand hygiene supplies for those entering the space
- Ensure adequate physical distancing from vaccinees to vaccinees throughout the entire process (>2 metres); at registration, while waiting to be immunized and during the post-vaccine observation period
- If possible, maintain unidirectional flow from entry to exit into the facility
Vaccine administration
- Administer vaccines in a clean space, with temporary or permanent barriers, adequately distanced from other vaccinees
- Ensure staff adhere to Infection Prevention & Control standards, including performing hand hygiene and wearing appropriate PPE
- If gloves are worn for the administration of the vaccine, they should be changed between vaccinees
- It is not necessary to wipe the skin prior to vaccine administration with alcohol or other cleaning solution[3]
Post Vaccine Observation
- Ensure there is adequate space for individuals to sit for the minimum 15 minute observation period post immunization
- Ensure that masks are worn and hand hygiene supplies is available as required
- High touch surfaces (eg. arms of chairs) should be cleaned with appropriate cleaning supplies (eg. hospital-grade disinfectant wipes) between use
This article initially appeared in the Globe and Mail on April 1, 2021.
[1] https://www.cdc.gov/niosh/topics/hierarchy/default.html
[2] https://www.cdc.gov/vaccines/pandemic-guidance/index.html?deliveryName=USCDC_7_3-DM34944
[3] Pakes BN, Taddio A. Wiping the alcohol swab away from COBID-19 vaccine program https://rsc-src.ca/en/voices/wiping-alcohol-swab-away-from-covid-19-vaccine-program


